Heroin Addiction: Signs, Symptoms, Risks, and Treatment Resources
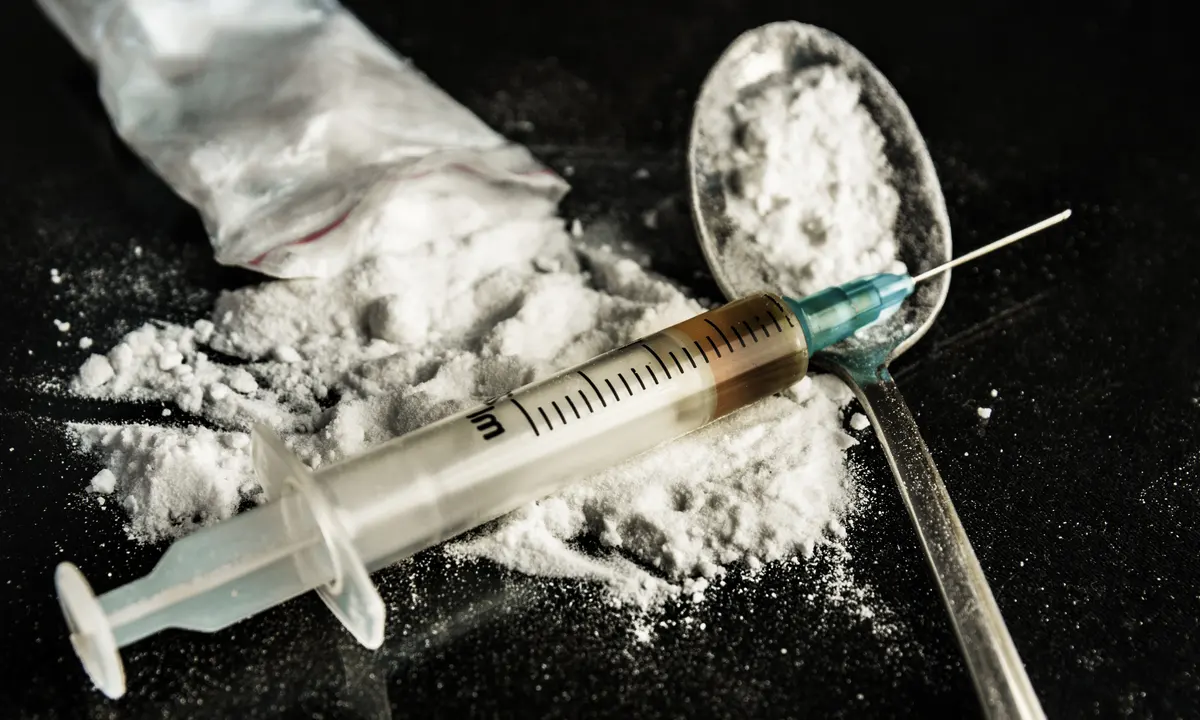
- Heroin is a potent, highly addictive opiate derived from opium poppies
- As a Schedule I drug in the United States, heroin is categorized as a substance that has a high potential for abuse and no currently accepted medical use in treatment
- Known for its signature rush of euphoria, heroin works on the opiate receptors of the brain
- Heroin may be injected, smoked, or snorted, and each of these methods of ingestion comes with risks
- Heroin overdoses can easily turn deadly due to the drug’s depressant effects on breathing, heart rate, and other essential bodily systems
- Naloxone can reverse the effects of a heroin overdose in the short term
- Heroin addiction is classified as an Opioid Use Disorder in the DSM-5
- Treatment for heroin addiction includes withdrawal management, psychological treatment, and long-term medications and lifestyle changes
What is Heroin?
Heroin is a highly potent opiate drug derived from the seed pod of several varieties of poppy plants. It may appear as a white or brown powder or in the form of a black sticky substance known as ‘black tar heroin.’ This central nervous system depressant is known for a euphoric rush which quickly takes larger doses to achieve.
Heroin Quick Reference
| Drug Category | Commercial & Street Names | DEA Schedule | Administration |
| Opioid | Black Pearl, Black Stuff, Black Eagle, Brown, Brown Sugar, Brown Tape, Chiba, Chiva, China White, Dope, Dragon, H, Hero, Horse, Junk, Scat, Skag, Smack, Tar, White Boy/Girl, Witch Hazel, White Horse, White Lady, Mexican Brown, Mexican Mud, Number 3/4/8 | Schedule I |
|
Heroin’s Effects on the Mind and Body
When heroin enters the body, it immediately activates opioid receptors in the brain. These receptors are responsible for modulating the experiences of pleasure and pain and are the reason for the instant euphoric rush that makes heroin so addictive. At the same time, heroin slows down the nervous system, resulting in a feeling of extreme relaxation.
How Does Heroin Affect the Brain?
When heroin activates opioid receptors in the brain, it not only induces feelings of euphoria but also inhibits the transmission of pain signals, contributing to its analgesic properties. As a result, the brain begins to flood with a much higher level of dopamine than what would ever occur naturally. Dopamine is a neurotransmitter that provides individuals with feelings of happiness, well-being, and satisfaction.
Heroin also alters an individual’s state of mind, with many users reporting:
- Clouded mental functioning
- A warm, calm feeling
- An increased feeling of well-being and confidence
How Does Heroin Affect the Body?
Heroin is a highly potent opioid derived from the seed pod of several varieties of poppy plants. This means it slows down critical bodily functions, including breathing, body temperature, blood pressure, and even heartbeats. Also, heroin overdoses have resulted in more than 17,000 deaths in the U.S. in 2021[1].
Heroin’s opioid effects may be experienced as follows:
- Warm flushing of the skin
- A heavy feeling in my arms and legs
- ‘Pinpoint’ or very constricted pupils
- Nausea and vomiting
- Severe itching
- Going ‘on the nod,’ a back-and-forth state of being conscious and semi-conscious
- Slowed breathing
- Slowed heart rate
What are the Long-Term Effects of Taking Heroin?
Heroin use spanning weeks, months, or years can have serious physical and mental health consequences. These depend on factors including the method of taking heroin, the dosage, and the individual’s pre-existing level of health. These long-term effects may include:
- Insomnia
- Infection of the heart lining and valves
- Constipation and stomach cramping
- Liver and kidney disease
- Lung complications, including chronic pneumonia
- Sexual dysfunction
- Irregular menstrual cycle for women
- Pervasive mental disorders, including depression and antisocial personality disorder
The Risks of Injecting Heroin
Intravenous injection of heroin puts individuals at risk of collapsed veins, skin abscesses, and serious bacterial infections and increases the risk of transmitting bloodborne diseases like HIV and hepatitis due to needle sharing.[2]
The Risks of Smoking Heroin
Smoking heroin is the second most common form of heroin consumption. This method increases the chances of potentially fatal coughing fits called bronchospasms. It also increases the likelihood of irreversible damage to the white matter in the brain, likely due to the chemicals in the aluminum.[3]
The Risks of Sniffing Heroin
Sniffing heroin may seem less dangerous than injecting it, but it comes with different risks. In addition to damaging the tissues of the nasal passage, it damages the structures that give the nose its shape. It also causes irritation and inflammation across the entire respiratory system.
The Dangers of A Heroin Overdose
One of the biggest risks of heroin is its potential for overdose. As a central nervous system depressant, heroin slows down essential bodily functions. In cases of overdose, this can result in breathing and heartbeat stopping completely within 2-3 minutes.
Heroin and Fentanyl
The risk of overdosing on heroin is amplified by the increasing saturation of fentanyl[4] and other contaminants in the drug supply. The risk of heroin overdose is significantly increased by the presence of fentanyl, a substance far more potent than heroin. Users often cannot detect its presence, dramatically elevating the risk of overdose.
How to Stop a Heroin Overdose
Naloxone, available as a nasal spray or injection, is an opioid antagonist that can reverse the life-threatening effects of a heroin overdose. Quick administration is crucial for restoring breathing and preventing death until emergency medical help arrives.[5]
Understanding Heroin Addiction
The reason heroin is highly addictive lies in the way it trains the brain. Like other opioids, heroin causes the neuron synapses to flood with an excess of naturally occurring endorphins and dopamine. But in a very short amount of time, the brain stops making these chemicals naturally, forcing individuals to rely on heroin for even a base level of comfort.
This internal impact is reflected in the numbers we see in our society, with an estimated 23% of individuals becoming addicted after trying heroin in 2014[6].
Diagnosing a Heroin Addiction
Heroin addiction is classified as an Opioid Use Disorder (OUD) according to the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5).
To confirm a diagnosis of Opioid Use Disorder (OUD), at least two of the following should be observed within a 12-month period:
- Opioids are often taken in larger amounts or over a longer period than was intended.
- There is a persistent desire or unsuccessful efforts to cut down or control opioid use.
- A great deal of time is spent in activities necessary to obtain the opioid, use the opioid, or recover from its effects.
- Craving, or a strong desire or urge to use opioids.
- Recurrent opioid use results in a failure to fulfill major role obligations at work, school, or home.
- Continued opioid use despite having persistent or recurrent social or interpersonal problems caused or exacerbated by the effects of opioids.
- Important social, occupational, or recreational activities are given up or reduced because of opioid use.
- Recurrent opioid use in situations in which it is physically hazardous.
- Continued opioid use despite knowledge of having a persistent or recurrent physical or psychological problem that is likely to have been caused or exacerbated by the substance.
- The users exhibit tolerance to opioids, requiring a markedly increased amount to achieve the desired effects.
- The user exhibits withdrawal symptoms.
Recovering from Heroin Addiction
Heroin addiction affects individuals from a huge variety of backgrounds and demographics, but they all have one thing in common — they can recover. Treatment for heroin addiction follows the same path as other Opioid Use Disorders. This includes withdrawal management, psychological treatment, long-term relapse prevention, and lifestyle maintenance.
Managing Heroin Withdrawal Symptoms
Heroin withdrawal involves challenging and unpleasant symptoms. These symptoms can be managed through medically assisted detoxification and the use of FDA-approved medications such as methadone and buprenorphine. Naltrexone is used primarily for maintaining abstinence after detoxification, rather than for managing acute withdrawal symptoms.
Early Heroin Withdrawal Symptoms
Some of the earliest symptoms of heroin withdrawal will show up within the first 8 to 24 hours and may include:
- Increased breathing rate and blood pressure
- Elevated body temperature and low fever
- A fast pulse and heartbeat
- Dilated pupils
- Unusually heightened reflexes
- Sweating
- Goosebumps
- Water discharge from eyes and nose
- Muscle pain and spasms, especially in the legs and back
- Bone pain
- Diarrhea, nausea, and vomiting
Long-Term Heroin Withdrawal Symptoms
After an initial short-term period of acute withdrawal from heroin, longer-term symptoms will show up. Typically these occur between 3-10 days after the last dose of this opiate and may include:
- Continued mood disorders, including pervasive dysphoria, depression, and anxiety, requiring additional treatment
- Heavy fatigue and exhaustion
- A loss of interest in activities
- Short-term memory problems
- Decreased attention, impaired concentration, and difficulty making decisions
- Drug craving
Psychological Treatment for Opioid Use Disorder
After withdrawal symptoms are manageable for an individual, the second stage of treatment can begin. This stage involves therapeutic and psychological interventions that help individuals understand the root of their heroin addiction and develop skills to avoid a relapse in the future.
The psychological treatment stage may occur as part of an inpatient or an outpatient program. One-on-one talk therapy, group therapy, and family addiction counseling will be paired with behavior skills training. The most common behavioral skills training methodologies for Opioid Use Disorder include Dialectical Behavioral Therapy (DBT) and Cognitive Behavioral Therapy (CBT).
Long-Term Lifestyle Maintenance for Opioid Use Disorder
Recovery from heroin addiction typically requires long-term medication for opioid use disorder (MOUD) along with ongoing outpatient counseling. Many individuals find attending a peer-led support group helpful, as it allows them to share challenges, share challenges, learn from others, and find social relationships that support continued recovery and sobriety.
Frequently Asked Questions
Are you or a loved one struggling with Heroine addiction?
